جراحی مغز و اعصاب
این مقاله دقیق، کامل و صحیح ترجمه نشده و نیازمند ترجمه از انگلیسی به فارسی است. کل یا بخشی از این مقاله به زبان انگلیسی نوشته شدهاست. اگر مقصود ارائهٔ مقاله برای مخاطبان زبان انگلیسی است، باید در ویکیپدیای انگلیسی نوشته شود (فهرست ویکیپدیاها را ببینید). در غیر این صورت، خواهشمند است ترجمهٔ این مقاله را با توجه به متن اصلی و با رعایت سیاست ویرایش، دستور خط فارسی و برابر سازی به زبان فارسی بهبود دهید و سپس این الگو را از بالای صفحه بردارید. همچنین برای بحثهای مرتبط، مدخل این مقاله در فهرست صفحههای نیازمند ترجمه به فارسی را ببینید. اگر این مقاله به زبان فارسی بازنویسی نشود، تا دو هفتهٔ دیگر نامزد حذف میشود و/یا به ویکیپدیای انگلیسی منتقل خواهد شد. اگر مایل به ارزیابی این مقاله هستید، میتوانید ترجمهٔ گوگل از این مقاله را ببینید. در هر حال، لطفاً ترجمهٔ ماشینی دیگری به این مقاله اضافه نکنید، چرا که این گونه از ترجمهها عموماً کیفیت بسیار پایینی دارند. |
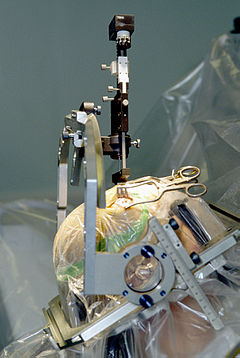 درج هدایتشده استریوتاکتیک الکترودهای DBS در جراحی مغز و اعصاب | |
| پیشه | |
|---|---|
زمینههای فعالیت | جراحی |
| توصیف | |
تحصیلات موردنیاز |
یا
یا
|
زمینه کاری | بیمارستانها، درمانگاهها |
جراحی مغز و اعصاب (به انگلیسی: Neurosurgery) یا (به انگلیسی: neurological surgery) یک رشتهٔ تخصصی و فوق تخصصی پزشکی است در رابطه با پیشگیری، تشخیص، درمان و توانبخشی اختلالاتی که بر هر بخش از دستگاه عصبی شامل مغز، نخاع، اعصاب پیرامونی و دستگاه عروق مغزی خارج از جمجمه تأثیرگذار است.[۱][۲][۳]
آموزش و فراگیری[ویرایش]
در کشورهای مختلف، ملزومات برای تمرین قانونی جراحی مغز و اعصاب، برای هر فردی متفاوت بوده و همچنین روش های آموزش دیدن و فراگیری این علم نیز فرق میکند. در بیشتر کشورها، جراحان مغز و اعصاب، به حداقل هفت سال آموزش دیدن پس از فارغ التحصیلی از دانشگاه علوم پزشکی نیاز دارند. [۴]
در ایران[ویرایش]
در این کشور بهطور کلی یک جراح مغز و اعصاب باید هفت سال در دانشگاه علوم پزشکی، پزشکی عمومی و پنج تا شش سال دستیاری ویژه را پشت سر بگذارد. [۵] بیشتر دورههای دستیاری بخشهای علوم پایه و پژوهشهای بالینی دارند. جراحان مغز و اعصاب ممکن است دورههای آموزشی بیشتری را پس از دورهٔ دستیاری یا در برخی موارد به عنوان یک دستیار ارشد با کمک هزینهٔ آموزشی پیگیری کنند. این دورههای آموزشی عبارتند از: جراحی مغز و اعصاب کودکان، مراقبت آسیب/اعصاب بحرانی، جراحی کارکردی و استریوتاکتیکی، عصب-سرطانشناسی وابسته به جراحی، پرتوجراحی، جراحی رشتههای عصبی (نوروواسکولار)، عصب پرتوشناسی مداخلهای، عصب پیرامونی، جراحی ستون فقرات و جراحی قاعدهٔ جمجمه. جراحان مغز و اعصاب همچنین میتوانند دورههای آموزشی آسیبشناسی عصبی (نوروپاتولوژی) و عصب-چشمپزشکی (نورو-اوفتالمولوژی) را با کمک هزینههای آموزشی بگذرانند. برای جراح شدن باید علاقه شخص بسیار زیاد باشد و توان طی کردن دورههای طاقت فرسا را داشته باشد.[۶]
در بریتانیا[ویرایش]
در بریتانیا دانش آموزان باید ورودی به دانشگاه علوم پزشکی را به دست بیاورند. دریافت مدرک تحصیلی امبیبیاس (کارشناسی پزشکی، کارشناسی جراحی) بسته به مسیر آموزشی دانشجو چهار تا شش سال به درازا میانجامد. سپس تازه پزشکان باید به مدت دو سال دوره آموزشی بنیادین را پشت سر بگذارند. این دوره یک دورهٔ پولی است که در یک بیمارستان طیف گستردهای از تخصصهای پزشکی از جمله جراحی را در بر میگیرد. سپس پزشکان تازهوارد برای ورود به یک دورهٔ عصبشناسی درخواست میکنند. برخلاف سایر رشتههای جراحی، این رشته دورهٔ آموزشی مستقل خود را دارد که حدود هشت سال به طول میانجامد.[۷]
روشهای عصب پرتوشناسی در تشخیص و درمان در جراحی مغز و اعصاب استفاده میشوند از جمله تصویربرداری به کمک رایانه یا مقطعنگاری رایانهای، تصویرسازی تشدید مغناطیسی (ام آر آی)، مقطعنگاری با نشر پوزیترون، مغز نگاری مغناطیسی و جراحی استریوتاکتیکی. برخی از روندها در جراحی مغز و اعصاب شامل استفاده از تصویرسازی تشدید مغناطیسی (ام آر آی) و تصویرسازی تشدید مغناطیسی کاربردی در حین عمل است.
ریزجراحی در بسیاری از جنبههای جراحیهای عصبی مورد استفاده قرار میگیرد. هنگام انجام جراحی دهانهپیوست (آناستومسیس) ریزرگها ریزبین (میکروسکوپ) مورد نیاز است. در برش آنوریس ریزنگر مورد نیاز است. در جراحی ستون فقرات با کمترین تهاجم از این فنون و روشها استفاده میشود. روند جراحیهای مانند دیسککتومی، لامینکتومی و کارگذاری دیسک مصنوعی به وجود ریزبین وابسته است.[۸]
جراحی درون بینی (آندوسکوپی) با حداقل تهاجم توسط جراحان اعصاب مورد استفاده قرار میگیرد. روشهایی مانند جراحی درون بینی (منظور درون نگری است) اندونازال (درون دماغ) برای درمان تومورهای هیپوفیز، کرانیوفارنژیوما، کوردوما و ترمیم نشت مایع مغزی نخاعی مورد استفاده قرار میگیرد. از درون بینی (آندوسکوپی) بطنی در موارد کیستهای کلویدی و نوروسیسترکوس استفاده میشود. روشهای درون بینی میتواند برای کمک به تخلیهٔ هماتوم و درمان درد عصب سهقلو به کار برده شود. اختلالات جمجمهای صورت و اختلال گردش مایع مغزی نخاعی توسط جراح اعصاب درمان میشود. همچنین بسته به شرایط جراحی پلاستیک و جراحی ناحیهٔ فک و صورت توسط جراح اعصاب انجام میشود. مواردی مانند ناهنجاری آرنولد-کیاری، کرانیوسینوستوس و نخاعگشادگی نیز به دست جراح اعصاب درمان میشود. به این کرانیوپلاستی گفته میشود.
جراحان مغز و اعصاب در پرتوجراحی استریوتاکتیک در کنار پرتو سرطانشناس در درمان تومور و ناهنجاری رگی (ای وی ام) نقش دارند. از روشهای پرتوجراحی مانند چاقوی گاما (گاما نایف)، سایبرنایف و جراحی Novalis Shaped Beam به کار برده میشود.[۹]
تاریخچه[ویرایش]
جراحی مغز و اعصاب، یا برشهای برنامه ریزی شده در سر برای تسکین درد، هزاران سال است که وجود دارد اما پیشرفتهای قابل توجه در آن متعلق به صدسال اخیر است.[۱۰]
بیماریها[ویرایش]
حالتها و بیماریها دیگری که توسط جراحان مغز و اعصاب درمان میشوند شامل موارد زیر هستند:
- فتق دیسک بین مهرهای
- تنگی مجرای نخاعی گردنی یا تنگی مجرای نخاعی کمری
- وجود آب در مغز
- آسیب سر (خونریزی مغزی، شکستگی جمجمه و…)
- آسیب به طناب نخاعی
- آسیب فیزیکی دستگاه عصبی پیرامونی
- عفونت
- تومورهای ستون فقرات، مغزی، طناب نخاعی و اعصاب پیرامونی
- خونریزیهای درون مغزی مانند خونریزی زیر عنکبوتیه، خونریزیهای درون سلولی و بین بافتی
- برخی از انواع مقاومت به دارو در صرع
- Some forms of movement disorders (advanced پارکینسون، chorea) – this involves the use of specially developed minimally invasive stereotactic techniques (functional, stereotactic neurosurgery) such as ablative surgery and deep brain stimulation surgery
- Intractable pain of cancer or trauma patients and cranial/peripheral nerve pain
- Some forms of intractable psychiatric disorders
- Vascular malformations (i.e. , arteriovenous malformations, venous angiomas, cavernous angiomas, capillary telangectasias) of the brain and spinal cord
- بیماری مویامویا
جراحان مغز و اعصاب مطرح[ویرایش]
- کاظم فتحی
- مجید سمیعی ( سمیعی ، جراح برتر مغز و اعصاب در جهان )
پانویس[ویرایش]
- ↑ «نسخه آرشیو شده». بایگانیشده از اصلی در ۵ نوامبر ۲۰۱۲. دریافتشده در ۲۴ ژوئیه ۲۰۱۲.
- ↑ «AANS - Patient Information». بایگانیشده از اصلی در ۳۱ اوت ۲۰۱۱. دریافتشده در ۲۴ ژوئیه ۲۰۱۲.
- ↑ «جراحی مغز». 2019/05/11. تاریخ وارد شده در
|تاریخ=را بررسی کنید (کمک) - ↑ "Brain Surgeon: Job Description, Salary, Duties and Requirements". Science. Retrieved 29 December 2019.
- ↑ «ABNS.org». بایگانیشده از اصلی در ۲۴ ژوئیه ۲۰۱۲. دریافتشده در ۲۴ ژوئیه ۲۰۱۲.
- ↑ «نسخه آرشیو شده». بایگانیشده از اصلی در ۲۱ ژوئن ۲۰۱۰. دریافتشده در ۲۴ ژوئیه ۲۰۱۲.
- ↑ "The society of British neurological surgeons". Archived from the original on 11 March 2012. Retrieved 11/03/2011.
{{cite web}}: Check date values in:|accessdate=(help) - ↑ «Cyber Museum of Neurosurgery». بایگانیشده از اصلی در ۲۵ آوریل ۲۰۱۲. دریافتشده در ۲۴ ژوئیه ۲۰۱۲.
- ↑ «Stereotactic Radiosurgery Program | UCLA Neurosurgery». بایگانیشده از اصلی در ۱۴ اوت ۲۰۱۲. دریافتشده در ۲۴ ژوئیه ۲۰۱۲.
- ↑ "Neurosurgery". Wikipedia (به انگلیسی). 2023-06-22.