سقط جنین
| سقط جنین | |
|---|---|
| تخصص | پزشکی زایمان |
| طبقهبندی و منابع بیرونی | |
| آیسیدی-۱۰ | O۰۴ |
| آیسیدی-۹-سیام | 779.6 |
| دادگان بیماریها | 4153 |
| مدلاین پلاس | 002912 |
| ئیمدیسین | article/۲۵۲۵۶۰ |
| پیشنت پلاس | سقط جنین |
سقط جنین (آپگانه، آبگانه یا آفگانه در فارسی) به معنی از دست رفتن محصول حاملگی (جنین یا رویان) قبل از هفته ۲۰ بارداری است ولی پزشکان بیشتر از این اصطلاحات برای توصیف هر گونه پایان حاملگی در سهماهه اول بارداری استفاده میکنند.
سقط جنین، به معنای پایان یافتن بارداری در هر مرحلهای است که زندگی نوزاد در جریان است، اگرچه غالباً به لحاظ فنی و تخصصی، خاتمه یافتن بارداری به واسطهٔ جراحی یا خارج کردن جنین یا رویان از رحم (قبل از آنکه قادر به ادامه حیات باشد) را سقط جنین میگویند. مرگ جنین اگر به صورت خود به خود رخ دهد به آن سقط خودبهخودی (ناخواسته) گفته میشود. کاندوم وسیله ای است که با استفاده کردن از آن میتوان از وقوع بارداریهای ناخواسته جلوگیری کرد تا کار به سقط جنین کشیده نشود. استفاده از این وسیله به افرادی که نمیخواهند صاحب بچه شوند توصیه اکید میشود.
مقدمه[ویرایش]
در کشورهای توسعه یافته، مدت مدیدی است که سقط جنین خود خواسته و قانونی به لحاظ پزشکی از امنترین فرایندها محسوب میشود.[۱] با این حال سقط جنین ناسالم (که توسط فرد، بدون آموزش مناسب یا خارج از محیطهای پزشکی انجام میشود) سالانه حدود ۷۰ هزار مرگ مادر و ۵ میلیون معلول، در سطح جهان به جا میگذارد.[۲] سالانه حدود ۴۲ میلیون سقط جنین انجام میشود که تخمین زده شدهاست که ۲۰ میلیون از آنها به شکلی ناسالم انجام شدهاست.[۲] چهل درصد زنان حاملهٔ جهان از داشتن امکانات درمانی و حق انتخاب برای سقط جنین محروم هستند.[۳] سقط جنین عمدی (خواسته) دارای سابقهٔ تاریخی طولانی است که توسط روشهای مختلفی چون سقطکنندههای گیاهی، استفاده از ابزار تیز، آسیب جسمانی، و دیگر روشهای سنتی انجام میشدهاست. علم پزشکی معاصر با بهرهگیری از داروها و روشهای جراحی، سقط جنین را راحت کردهاست. قانونی بودن، همهگیر بودن، وضعیت فرهنگی، و وضعیت مذهبی در نوع نگاه به سقط جنین، تفاوت قابل ملاحظهای ایجاد میکند. در بسیاری از نقاط جهان، بحثهای جنجالی بر سرِ قانونی و اخلاقی بودن، سقط جنین وجود دارد. از آنجایی که دسترسی به آموزش و خدمات تنظیم خانواده برای پیشگیری از بارداری در سراسر جهان، در حال افزایش است، سقط جنین بهطور گستردهای در حال کاهش است.[۴]
تاریخچه[ویرایش]
سقط جنین خود خواسته دارای سابقهٔ طولانیای میباشد و میتوان ردههایی از آن را در تمدنهای مختلفی چون چین در زمان شننونگ (۲۷۰۰ قبل از میلادی)، مصر باستان در زمان ابریهای پاپیروس (۱۵۵۰ قبل از میلاد) و امپراطوری روم در زمان جوونال (۲۰۰ قبل از میلاد) یافت. شواهد نشان میدهد که سقط جنین از طریق روشهایی چون گیاهان، ادوات تیز، استفاده از فشارهای شکمی و روشهای دیگر انجام میشدهاست. برخی از محققان پزشکی و مخالفان سقط جنین خاطر نشان میکنند که سوگند دانشجویان پزشکی در یونان باستان، آنها را از انجام سقط جنین منع میکردهاست.[۵] با این حال دستهای دیگر از پژوهشگران با این تفسیر مخالفند[۵] متون پزشکی مربوط به طب بقراط، حاوی شرح روشهای نافرجام و یادداشتهایی مربوط به خطرات ناشی از سقط جنینِ ناامن است.[۶] در مسیحیت، پاپ (۹۰–۱۵۸۵) به عنوان اولین پاپ اشاره کرد که سقط جنین بدون در نظر گرفتن اینکه در چه مرحلهای از حاملگی باشد، قتل محسوب میشود.[۷] کلیسا قبلاً بر سر اینکه آیا سقط جنین قتل محسوب میشود یا نه، مجزا شده بود و مخالفت با سقط جنین تا قرن ۱۹، بهطور سرسختانهای ادامه داشت.[۸] سقط جنین در اسلام تا زمانی مجاز است که به اعتقاد مسلمانان روح در جنین دمیده نشده باشد.[۹] در زمانِ دمیده شدن روح در جنین، بین متکلمان اختلاف وجود دارد، عدهای معتقدند این زمان ۴۰ روز بعد از لقاح است و عدهای دیگر این زمان را ۱۲۰ روز بعد از لقاح در نظر گرفتهاند.[۹] با این حال سقط جنین عمدتاً در مناطق اسلامی با اعتقاد بالا همچون محدودهٔ خاورمیانه و شمال آفریقا، بهشدت محدود میشود یا اینکه ممنوع است. پیشرفت تکنیکهای سقط جنین در اروپا و آمریکا، از قرن ۱۷میلادی آغاز شد. با این وجود، محافظهکاری اغلب پزشکان در رابطه با مسایل جنسی، از گسترش وسیع تکنیکهای امن سقط جنین جلوگیری به عمل آورد.[۸] برخی پزشکان به تبلیغ خدمات خود دست زدند و فعالیتهای آنان تا قرن ۱۹ یعنی زمانی که سقط جنین هم در آمریکا و هم در بریتانیا ممنوع شد، تحت کنترل و نظارت گسترده قرار نداشت.[۱۰] گروههای مرتبط با کلیسا و نیز پزشکان در جنبشهای ضدِ سقطِ جنین شدیداً تأثیرگذار بودهاند.[۸] در آمریکا، تا حدود ۱۹۳۰ سقط جنین از زایمان به مراتب خطرناکتر بود، در این زمان بهبود فزاینده شیوههای سقط جنین نسبت به زایمان، موجب امنتر شدن سقط جنین میشد[یادداشت۴]. اتحاد جماهیر شوروی (۱۹۱۹)، ایسلند (۱۹۳۵) و سوئد (۱۹۳۸) از اولین کشورهایی بودند که برخی یا همه اشکال سقط جنین را قانونی کردند.[۱۱] در آلمانِ نازیِ ۱۹۳۵، قانونی تصویب شد که به موجب آن سقط جنین برای کسانی که «بهطور ارثی بیمار» تلقی میشدند، مجاز شمرده میشد، در حالیکه زنانی که به نژاد آلمان تعلق داشتند، به ویژه، از سقط جنین منع میشدند.[۱۲]
انواع[ویرایش]
سقط جنین عمدی (خودخواسته)[ویرایش]
هرسال در جهان حدود ۲۰۵ میلیون بارداری اتفاق میافتد. بیش از یک سوم آنها ناخواسته هستند و در حدود یک پنجم به سقط جنین عمدی ختم میشوند.[۱۳] بیشتر سقطها ناشی از بارداریهای ناخواسته میباشند.[۱۴] یک بارداری میتواند بهطور خودخواسته به شیوههای گوناگون به سقط جنین بینجامد. شیوهٔ انتخاب شده معمولاً به سن رویان یا جنین وابستهاست،[۱۵] که اندازهاش در جریان بارداری رشد میکند.[۱۶] همچنین ممکن است روشهای ویژهای با توجه به قانون، دسترس پذیری در منطقه، و ترجیح پزشک یا بیمار انتخاب گردد. دلایل انجام سقطهای عمدی:
- درمانی سقط در پزشکی هنگامی درمانی گفته میشود که برای حفظ جان زن باردار، پیشگیری از آسیب به سلامت جسمی یا روحیِ زن، دلالت نشانهها بر بالا بودن احتمال ابتلای جنین به بیماری یا مرگ پیشرس یا معلولیت، یا کاهش انتخابی تعداد جنینها به منظور پایین آوردن احتمال خطر برای سلامت جنین در بارداریهای چندگانه انجام شود.[۱۶]
- انتخابی سقط انتخابی یا داوطلبانه سقطی است که بنا به خواستِ زن به دلایل غیرپزشکی به دست خود یا دیگری انجام شده باشد.[۱۷]
سقط جنین غیرعمدی (ناخواسته)[ویرایش]
سقط جنین ناخواسته یا غیرعمدی، خروج ناخواسته رویان یا جنین پیش از هفتهٔ بیستم تا بیست و دوم بارداری است∗. چنانچه بارداری پیش از سی و هفت هفته خاتمه یابد و منجر به تولد نوزادی زنده گردد، «تولد زودرس»∗ یا «پیش از موعد»∗ تلقی میشود.[۱۸] جنینی که پس از حیات یافتن، در رحم یا در زمان وضع حمل بمیرد، عموماً با اصطلاح «جنین مرده به دنیا آمد»∗ شناخته میشود.[۱۹] تولد پیش از موعد و زایمانِ جنین مرده، عموماً سقط جنین تلقی نمیشوند، اگرچه استفاده از این اصطلاحات گاهی با یکدیگر همپوشانی پیدا میکند. تنها۳۰ تا ۵۰ ٪ از لقاحها، سهماهه اول را با موفقیت پشت سر میگذارند،[۲۰] حجم قابل توجهی از آن دسته از لقاحها که به ثمر نمیرسند، پیش از آنکه زن از عمل لقاح مطلع شده باشد، از بین میروند[۲۱] و بسیاری از بارداریها پیش از آنکه پزشکان توانایی تشخیص رویان را داشته باشند خاتمه مییابند.[۲۲] در بررسی از حداقل ۵۰ ٪ از بارداریهای زود خاتمه یافته، شایعترین دلیل سقط جنینِ غیرعمدی در طول سهماهه اول بارداری، اختلالات کروموزومی است[۱۰][۱۶]، از جمله سایر دلایل میتوان به بیماریهای عروقی (همچون لوپوس)، دیابت، سایر مشکلات هورمونی، عفونت و اختلالات رحمی اشاره کرد.[۲۳] بالا رفتن سن مادری و سابقه بیمار در سقط غیرعمدی جنین، به عنوان دو عامل اساسی مرتبط با افزایشِ ریسکِ سقطِ غیرعمدی شناخته میشوند.[۲۴] سقط جنین غیرعمدی، همچنین ممکن است در نتیجه تروما یا ضربه اتفاقی نیز رخ دهد.[۲۵]
ایمنی سقط جنین[ویرایش]
خطرات بهداشتی سقط جنین بستگی به این دارد که آیا روش انجام، بدون خطر یا غیربهداشتی است. سازمان جهانی بهداشت سقط جنین ناامن را روشی تعریف میکند که افراد غیر ماهر، با وسایل خطرناک یا در مراکز غیر بهداشتی انجام میدهند.[۲۶] سقط جنینی که در کشورهای توسعه یافته مطابق با قوانین انجام میشود، جزو کم خطرترین عملهای پزشکی است.[۲۷] در ایالات متحده، خطر مرگ مادران از سقط جنین ۰٫۵۶ در هر صدهزار سقط جنین است و حدود ۱۲٫۵ بار امن تر از زایمان (۷٫۰۶ مرگ و میر مادران در هر صدهزار تولد زنده) میباشد.[۲۸] خطر مرگ و میر مرتبط با سقط جنین با افزایش سن حاملگی افزایش مییابد، اما هنوز پایینتر از زایمان در ۲۱ هفتگی حاملگی است.[۲۹][۳۰]
روشها[ویرایش]
- آسپیراسیون خلاء∗ در سهماهه اول امنترین روش سقط جراحی است و میتواند در یک مطب مراقبتهای اولیه، کلینیک سقط جنین، یا بیمارستان انجام شود. عوارض نادر هستند و میتواند سوراخ شدگی رحم، عفونت لگن خاصره، ماندن جفت و نیاز به تخلیه مجدد باشد.[۳۱] آنتیبیوتیک پیشگیرانه (مانند داکسی سیکلین یا مترونیدازول) بهطور معمول قبل از سقط جنین انتخابی داده میشود،[۳۲] چون اعتقاد بر این است که بهطور قابل ملاحظهای خطر عفونت پس از عمل رحم را کاهش میدهد.[۳۳] عوارض پس از سقط سهماهه دوم شبیه به عوارض افرادی است که بعد از سهماهه اول سقط میکنند و تا حدودی به روش انتخاب شده بستگی دارد.
- اتساع و تخلیه∗ بررسی کتابخانهای کوکران در سال ۲۰۰۸ نشان داد که اتساع و تخلیه از روشهای دیگر سقط در سهماهه دوم امنتر بود.[۳۴]
- سقط دارویی سقط دارویی با میفه پریستون و میزوپروستول پس از ۴۹ روز از سن حاملگی مؤثر است.[۳۵] در زنان تا ۶۳ روز پس از سن حاملگی استفاده شدهاست، البته با افزایش خطر عدم موفقیت (با نیاز به سقط جنین جراحی)[۳۶] سقط جنین دارویی به اندازه سقط جنین جراحی در سهماهه اول، امن است، اما همراه با درد بیشتر و موفقیت کمتر است.[۳۷] به بهطور کلی، خطر عفونت رحم، به روش دارویی از سقط جراحی کمتر است،[۳۸] هر چند در سال ۲۰۰۵ چهار مورد مرگ و میر پس از سقطهای دارویی، ناشی از عفونت با کلستریدیوم سوردلی گزارش شدهاست.[۳۹] پس از این، برخی از ارائه دهندگان سقط جنین استفاده از آنتیبیوتیک پیشگیرانه را همراه با سقط دارویی شروع کردهاند.[۴۰]
سقط جنین ناامن علت عمدهای از آسیب و مرگ در میان زنان در سراسر جهان است. اگر چه دادهها مبهم هستند، تخمین زده میشود که سالانه حدود ۲۰ میلیون سقط جنین نا امن انجام میشوند، که ۹۷ ٪ آن در کشورهای در حال توسعه رخ میدهد.[۱] نتیجه سقط جنین غیربهداشتی، سالانه حدود ۶۸۰۰۰ مرگ و میر[۴۱] و میلیونها آسیب است.[۴۲] اعتقاد بر این است که شرایط قانونی سقط جنین نقش عمدهای در میزان سقط جنین ناامن دارد.[۴۳][۴۴] به عنوان مثال، در سال ۱۹۹۶ قانونی کردن سقط جنین در آفریقای جنوبی تأثیر مثبت و فوری، حدود ۹۰ درصد کاهش، در میزان عوارض مرتبط با سقط جنین،[۴۵] و مرگ و میر ناشی از سقط جنین داشت.[۴۶] سازمان بهداشت جهانی با تأکید بر قانونی کردن سقط جنین، آموزش پرسنل پزشکی، و حصول اطمینان از دسترسی به خدمات بهداشت باروری از رویکرد سلامت عمومی حمایت میکند.[۴۴]
فرضیه سرطان پستان[ویرایش]
برخی مطالعات ارتباط بین سقط و سرطان پستان را نشان دادهاند.[۴۷] طرفداران ارتباط علیتی بین این دو معتقدند که وقفه در رشد طبیعی پستان در دوران بارداری سلولهای نابالغی را ایجاد میکند که بیشتر مستعد سرطان در سینهاست. با این حال، جامعه علمی پس از بررسی شواهد و تحقیقات دقیق نتیجه گرفتهاست که چنین ارتباطی وجود ندارد. نهادهای مهم پزشکی، از جمله سازمان بهداشت جهانی، مؤسسه ملی سرطان ایالات متحده، انجمن سرطان و… همه به این نتیجه رسیدند که سقط جنین، سرطان پستان ایجاد نمیکند.[۴۸] مفهوم یک ارتباط علیتی بین سقط جنین عمدی و سرطان پستان در حال حاضر عمدتاً توسط گروههای طرفدار زندگی ترویج میشود.[۴۷]
بهداشت روانی[ویرایش]
توافق کنونی علمی بر آن است که هیچ رابطه علت و معلولی بین سقط جنین و مشکلات سلامت روانی وجود ندارد. انجمن روانشناسی آمریکا بر اساس شواهد علمی موجود، به این نتیجه رسیدهاست که یک مرتبه سقط جنین تهدیدی برای بهداشت روانی زنان نیست، و مشکلات سلامت روانی در این زنان بعد از سقط در سهماهه اول بیشتر از مشکلات پس از حاملگی ناخواسته نیست.[۴۹][۵۰] برخی مطالعات با نتیجهگیری فوق مخالف است، و معتقد است که افزایش قابل توجهی در مشکلات روحی و روانی پس از سقط وجود دارد. با این حال، این مطالعات به دلیل نادیده گرفتن سابقه اختلالات روانی، شدت یا عدم هرگونه از این اختلالات، یا انتخاب نادرست گروههای شاهد به دلیل نادیده گرفتن متغیرهای مداخله گر در آنها از سوی پژوهشگران و سازمانهای حرفهای مورد انتقاد قرارگرفتهاند.
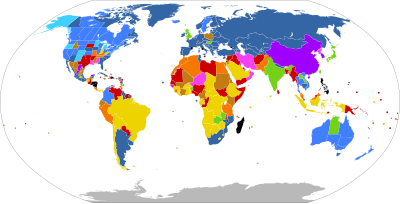
| قانونی در صورت درخواست | |
| بدون محدودیت | |
| محدودیت بارداری بعد از ۱۷ هفته اول | |
| محدودیت بارداری قبل ۱۷ هفته اول | |
| محدودیتهای نامشخص | |
| از نظر قانونی محدود به موارد زیر است: | |
| خطر برای زندگی مادر، برای سلامتی او *، تجاوز جنسی *، اختلال جنین *، یا عوامل اجتماعی و اقتصادی | |
| خطری برای زندگی مادر، برای سلامتی او *، تجاوز جنسی، یا اختلال در جنین | |
| خطر برای زندگی مادر، برای سلامت او *، یا آسیب جنین | |
| خطر جانی برای مادر *، سلامت *، یا تجاوز جنسی | |
| خطری برای زندگی یا سلامتی مادر | |
| خطری برای زندگی مادر | |
| غیر قانونی بدون استثنا | |
| بدون اطلاعات | |
| * برای برخی از کشورها یا مناطق در آن دسته اعمال نمی شود | |
میزان سقط جنین[ویرایش]
تعداد سقط جنین انجام شده در سراسر جهان بین سالهای ۱۹۹۵ و ۲۰۰۳ از ۴۵ میلیون به ۴۱ میلیون نفر کاهش یافتهاست، که به معنی کاهش در میزان سقط جنین از ۳۵ به ۲۹ در هر ۱۰۰۰ زن است. بیشترین کاهش در کشورهای توسعه یافته با کاهشی از ۳۹ به ۲۶ در هر ۱۰۰۰ زن در مقایسه با کشورهای در حال توسعه، که کاهشی از ۳۴ به ۲۹ در هر ۱۰۰۰ زن رخ دادهاست. از مجموع حدود ۴۲ میلیون سقط جنین، ۲۲ میلیون ایمن رخ دادهاست و ۲۰ میلیون مخفیانه و غیربهداشتی است.[۲] بهطور میانگین، فراوانی سقط جنین در کشورهای در حال توسعه (که در آن سقط جنین بهطور کلی محدود است) به فراوانی در کشورهای توسعه یافته (که در آن سقط جنین بهطور کلی بسیار کمتر محدود است) شباهت دارد.[۵۱][۵۲] اندازهگیری میزان سقط جنین در مکانهایی که سقط جنین در آنها غیرقانونی هستند، بسیار دشوار است به عقیده مؤسسه گات ماچر و صندوق جمعیت سازمان ملل متحد، میزان سقط جنین در کشورهای در حال توسعه تا حد زیادی به علت عدم دسترسی به روشهای ضدبارداری مدرن میباشد؛ با فرض هیچ تغییری در قوانین سقط جنین، با دسترسی به روشهای ضدبارداری سالانه حدود ۲۵ میلیون سقط جنین کمتر رخ میدهد، از جمله تقریباً ۱۵ میلیون کمتر سقط جنین ناامن.[۵۳] بروز سقط جنین عمدی به صورت منطقهای متفاوت است. برخی از کشورها، از جمله بلژیک (۱۱٫۲ از ۱۰۰ حاملگی شناخته شده) و هلند (۱۰٫۶ در ۱۰۰)، نسبت پایینی از سقط جنین عمدی داشتهاند. برخی دیگر مانند روسیه (۶۲٫۶ از ۱۰۰) رومانی (۶۳ از ۱۰۰)[۵۴] و ویتنام (۴۳٫۷ از ۱۰۰) نسبتی بالا داشتهاند (دادههای سه کشور اخیر کاملاً مجهول است). نسبت جهانی تخمین زده شده ۲۶ درصد بود، میزان جهانی—۳۵ در هر ۱۰۰۰ زن.[۵۵]
- به تازگی یک پژوهش نشان دادهاست که میزان انجامِ سقطجنین در کشورهای مختلف، صرفنظر از اینکه در آنها سقطجنین امری قانونی است یا نه یکسان است. تفاوت عمده بین کشورهایی که سقط در آنها قانونی است و کشورهایی که سقط در آنها به شدت ممنوع است در این است که در کشورهای دستهٔ اول، سقطجنین در شرایطی از نظر پزشکی ایمن و بیخطر صورت میگیرد در حالیکه در کشورهای دستهٔ دوم که سقط امری غیرقانونی است معمولاً این عمل در شرایطی از نظر پزشکی ناایمن صورت میگیرد. این در حالیست که سالانه دهها هزار زن، به دلیلِ دشواریها و مشکلاتِ ناشی از سقطهای انجامشده به روشِ ناایمن و غیربهداشتی جان خود را از دست میدهند.[۵۶]
- میزان انجام سقطجنین با میزان دسترسی به روشهای کنترلِ بارداریِ کارآمد «همبستگی» دارد، به شکلی که هرچه در کشوری ابزارهای کنترل بارداری کمتر در دسترس باشد، میزانِ انجام سقطجنین بالاتر است. همانطور که در یک مقاله عنوان شدهاست، «سریعترین راه برای کاهشِ میزانِ سقطجنین، فراهمکردنِ ابزارهای پیشگیری از بارداریِ قابل اعتماد است.»[۵۶]
- براساس آمار جهانی میزان شیوع سقط مکرر جنین ۳ تا ۴ درصد کل بارداریها است. سقط مکرر علل مختلفی دارد که از جمله آنها میتوان به عوامل ژنتیکی اشاره کرد که عامل بروز ۵ تا ۱۰ درصد سقطهای مکرر و ۶۰ تا ۷۰ درصد کل سقطها در جهان محسوب میشود.[۵۷]
سن حاملگی و روش آن[ویرایش]
میزان سقط جنین به مرحله بارداری و روش انجام آن بستگی دارد. در سال ۲۰۰۳، مراکز کنترل و پیشگیری بیماری (CDC) گزارش کرد که ۲۶ ٪ از سقط جنینها در حاملگی کمتر از ۶ هفته، ۱۸ درصد در ۷ هفته، ۱۵ درصد در ۸ هفته، ۴٫۱ درصد در ۱۶ … تا۲۰ هفته و ۱٫۴ ٪ در بیش از ۲۱ هفته رخ دادهاست. ۹۰٫۹ ٪ از سقطها از طریق «کورتاژ» (مکش- آسپیراسیون، اتساع و کورتاژ، اتساع و تخلیه)، ۷٫۷ ٪ به وسیلهٔ دارو (میفه پریستون)، ۰٫۴ ٪ با «تزریق داخل رحمی» (محلول نمکی یا پروستاگلندین)، و ۱٫۰ ٪ از طریق «روشهای دیگر» (از جمله سزارین و هیسترکتومی) انجام شدهاست.[۵۸] طبق نظر CDC، با توجه به مشکلات جمعآوری اطلاعات، دادهها باید به صورت تجربی مشاهده گردند و برخی از مرگ و میرهای جنین در بیش از ۲۰ هفتگی ممکن است مرگ و میر طبیعی باشند که به خاطر خارج نمودن جنین با همان روش سقط جنین عمدی[۵۹] به اشتباه تحت عنوان سقط جنین گزارش شدهاند. مؤسسه گات ماچر ۲۲۰۰ مورد اتساع کامل و تخلیه مکشی را طی سال ۲۰۰۰ در ایالات متحده برآورد کردهاست، این تعداد ۰٫۱۷ ٪ از تعداد کل سقط جنین انجام شده در آن سال است.[۶۰] بهطور مشابه در انگلستان و ولز در سال ۲۰۰۶، ۸۹ درصد از سقطها در ۱۲ هفتگی یا کمتر از آن، ۹ درصد بین ۱۳ تا ۱۹ هفتگی، و ۱٫۵ ٪ در بیش از ۲۰ هفتگی بارداری انجام شدهاست. ۶۴ ٪ از سقطهای گزارش شده به روش دمیدن هوا، ۶ درصد توسط E & D، و ۳۰ ٪ دارویی بود.[۶۱]
عوامل شخصی و اجتماعی[ویرایش]
مطالعهای که در سال ۱۹۹۸ در ۲۷ کشور دربارهٔ دلایل زنان برای خاتمه بارداری انجام شد نشان داد شایعترین دلیل زنان برای سقط جنین، به تعویق انداختن بچه دار شدن به زمان مناسب تر یا تمرکز قوا و منابع بر روی کودکان موجود بود. شایعترین دلایل عوامل اجتماعی - اقتصادی بودند مانند ناتوانی در پرداخت هزینه کودک از جمله هزینههای مستقیم برای تربیت فرزند یا از دست دادن درآمد هنگام مراقبت از فرزند، عدم حمایت از سوی پدر، عدم توانایی مالی برای داشتن کودکان اضافی، تمایل به ارائه تحصیل برای کودکان موجود، اختلال در تحصیل، مشکلات رابطه با شوهر و ذکر این که او بیش از حد جوان و بیکار است.[۶۲] مطالعهای در سال ۲۰۰۴ که در آن زنان آمریکایی در کلینیکی پرسشنامهای را پاسخ دادند نتایج مشابهی داشت.[۶۳] بررسی سال ۱۹۹۸ خطر برای سلامت مادران را دلیل اصلی با نسبت ۵–۱۰ درصد در هفت کشور و ۲۰–۳۸ ٪ در سه کشور (کنیا، بنگلادش و هند) عنوان کرد.[۶۲] در گزارش ۱۹۹۷ ایالات متحده، سلامت مادران «مهمترین دلیل» ۳٪ از زنان و نگرانی از سلامت جنین دلیل ۳٪ دیگر عنوان شد.[۶۴] در سال ۲۰۰۴ در نظر سنجی در آمریکا ۱٪ از زنانی که سقط جنین داشتند در نتیجه تجاوز باردار شده بودند و ۰٫۵ ٪ در اثر زنای با محارم.[۶۳] مطالعهای در سال ۲۰۰۲ در آمریکا به این نتیجه رسید که ۵۴ ٪ از زنانی که سقط جنین داشتند هنگام باردار شدن از یکی از روشهای ضدبارداری استفاده میکردند در حالیکه ۴۶ ٪ از این روشها استفاده نمیکردند. ۴۹ ٪ از افراد از کاندوم، استفاده ناپایدار و ۷۶ ٪ از آنها قرص ضد حاملگی خوراکی ترکیبی مصرف کرده بودند؛ ۴۲ ٪ از کسانی که کاندوم استفاده کرده بودند عدم موفقیت را در نتیجه لغزش یا پارگی عنوان کردند.[۶۵] مؤسسه گات ماچر تخمین زدهاست که "اکثر سقط جنینها را در ایالات متحده زنان اقلیتها انجام میدهند "چون زنان اقلیت "میزان بسیار بالاتری از بارداری ناخواسته دارند."[۶۶] برخی از سقط جنینها در نتیجه فشارهای اجتماعی است. از جمله ندادن حق به افراد معلول برای داشتن فرزند، اولویت برای کودکانی از جنس خاص، تقبیح مادران مجرد، حمایت اقتصادی ناکافی از خانوادهها، عدم دسترسی یا نفی روشهای پیشگیری از بارداری یا تلاش در جهت کنترل جمعیت (مانند سیاست تک فرزندی در چین). گاهی اوقات این عوامل میتواند به سقط جنین اجباری یا سقط جنین جنس انتخابی منجر شود.
رابطهٔ سقط جنین و بزهکاری[ویرایش]
به دنبال قانونیشدن سقطجنین در ایالات متحده در اوایل دههٔ ۱۹۷۰، میزانِ بزهکاری در این کشور بهطور ناگهانی و جدی کاهش یافت. این کاهش در حولوحوش سال ۱۹۹۰ ظاهر شد، یعنی ۱۷ سال پس از قانونیشدن سقطجنین در این کشور. البته اینکه کودکانِ ناخواسته، غالباً تبدیل به بزرگسالانی ناتوان [و در نتیجه غالباً مشکلدار و مشکلساز] میشوند از مدتها قبل شناخته شده بود. با اینکه وجود «همبستگی» بین دو «متغیر»، لزوماً نشاندهندهٔ «رابطهٔ علی» بین آن دو نیست اما برخی دانشمندان علوم اجتماعی، با تحلیل آماری حجمِ بالایی از دادهها به این نتیجه رسیدهاند که در دسترس بودن امکانِ سقطجنین، فاکتور مهمی در کاهشِ متعاقب در میزانِ بزهکاری بودهاست.[۵۶]
سقط جنین ناامن (غیر بهداشتی)[ویرایش]
گاهی اوقات زنان برای خاتمه دادن به دورهٔ بارداری خود به شیوههای ناامن متوسل میشوند، به خصوص زمانی که عمل سقط جنین، محدودیت قانونی نیز بههمراه داشته باشد. حدود یک مورد از هشت مرگ و میر مرتبط با حاملگی، در سراسر جهان، به سقط جنین ناامن مربوط میشود.[۶۷] تعریف سازمان بهداشت جهانی(WHO) از سقط جنین ناامن "روش انجام عمل سقط جنین توسط افراد فاقد مهارتهای لازم ویا انجام این عمل در محیطهایی با حداقل استانداردهای پزشکی یا دارا بودن هر دو این شرایط "است.[۶۸] سقط جنین ناامن ممکن است از طریق خود زن یا توسط فرد دیگری بدون آموزشهای پزشکی، یا توسط عامل حرفهای در محیطی با شرایطی زیر استانداردهای لازم انجام بگیرد. قانونی بودن سقط جنین یکی از عوامل اصلی ایمنی آن است. محدودیتهای قانونی مربوط به سقط جنین با نرخ بالایی از سقط جنینهای ناامن همراه است.[۲][۶۹][۷۰] علاوه براین، عدم دسترسی به راههای امن و مؤثر پیشگیری از بارداری، منجر به سقط جنین ناامن میشود. برآورد شدهاست که اگر برنامههای مربوط به تنظیم خانواده و خدمات بهداشتی، در سطح جهانی، به راحتی قابل دسترس خانوادهها باشد، بروز سقط جنین ناامن میتواند ۷۳ درصد کاهش یابد، بدون آنکه تغییری در محدودیتهای قانونی مربوط به سقط جنین ایجاد شود.[۷۱] چهل درصد زنان جهان قادرند به امکانات درمانی و انتخابی سقط جنین در دوره حاملگی دسترسی پیدا کنند.[۳] در حالی که به ندرت در سقط جنین امن مرگ و میر یافت میشود، ۷۰۰۰۰ مرگ و میر و ۵ میلیون معلولیت در هر سال، نتیجه سقط جنین ناامن است.[۷۲] عواقب مربوط به سقط جنین در حدود ۱۲ درصد مرگ مادران در آسیا، ۲۵ درصد در آمریکای لاتین و ۱۳ درصد در کشورهای جنوب صحرای آفریقا، محاسبه شدهاست.[۷۳] تخمین زده شدهاست که حدود ۲۴ میلیون زن دچار ناباروری ثانویهٔ ناشی از سقط جنین ناامن میشوند.[۷۴] اگر چه نرخ جهانی سقط جنین از ۶/۴۵ میلیون نفر در سال ۱۹۹۵ به ۶/۴۱ میلیون نفر در سال ۲۰۰۳ کاهش یافتهاست، با این حال روشهای ناامن همچنان ۴۸٪ کل روشهای سقط جنین انجام شده در سال ۲۰۰۳ را تشکیل میدادند.[۷۵] دسترسی به برنامههای تنظیم خانواده، آموزش بهداشت، و بهبود در مراقبتهای بهداشتی در طول و بعد از سقط جنین توصیه میشود تا به درستی به این پدیده رسیدگی شود.[۷۶]
قوانین جدید سقط جنین[ویرایش]
در حال حاضر قوانین مربوط به سقطجنین متفاوت هستند. در سرتاسر جهان حساسیتهای مذهبی، اخلاقی و فرهنگی در تلاشند تا قوانین سقط جنین را تحت تأثیر خود قرار دهند. حق زندگی، حق آزادی و حق باروری سالم موارد عمدهٔ حقوق بشری هستند که گاهی اوقات به عنوان توجیهی برای وجود یا عدم وجود قوانین سقط جنین استفاده میشوند. در حوزههای قضائی که سقط جنین قانونی است، قبل از سقط جنین میبایست الزاماتی رعایت شوند. این الزامات معمولاً وابسته به سن جنین میباشند، در این رابطه یکی از دورههای سهماههٔ بارداری مورد بررسی قرار میگیرد. در مواقع ضروری محدودیتهای بسیاری لغو میشوند. برخی از حوزههای قضائی، در مواردی اینچنینی، قبل از اعمال قانون باید برای مدتی در انتظار بمانند: جهت تکمیل شدن اطلاعات در رابطه با رشد جنین یا تماس با پدر و مادر متقاضی جوانی که درخواست سقط جنین کردهاست.[[۷۷] حوزههای قضائی دیگر ممکن است از زن، رضایت پدر جنین را مطالبه کنند. این گروه از دستاندرکاران، بیماران را از خطرات احتمالیای که در فرایند سقط جنین محتمل است، آگاه میکنند، و مقامات پزشکی هم تصدیق میکنند که سقط جنین یا با روش طبی انجام میگیرد یا الزامی اجتماعی دارد. دیگر حوزههای قضایی بهطور کامل سقط جنین را ممنوع کردهاند. با این حال، بسیاری، اما نه همه، در مواردی همچون تجاوز جنسی، زنای با محارم، یا خطر حیات و سلامتی زن باردار، سقط جنین مجاز است. در کشورهایی که در آنها سقط جنین بهطور کامل ممنوع شدهاست، مانند نیکاراگوئه، میتوان به افزایش مرگ مادران که بهطور مستقیم یا غیرمستقیم ناشی از بارداری میباشد، اشاره کرد.[۷۸][۷۹] در برخی از کشورها مانند بنگلادش که سقط جنین بهطور اسمی ممنوع شدهاست، همچنین ممکن است درمانگاهها سقط جنین را در قالب خدمات بهداشت و درمانی مربوط به مشکلات دورهٔ قاعدگی، انجام دهند.[۸۰] در جاهایی که سقط جنین غیرقانونی است یا اینکه انگ اجتماعی سنگینی به همراه دارد، زنان باردار ممکن به گردشگری پزشکی روی آورند و به کشورهایی سفر میکنند تا در آنجا بتوانند به بارداری خود خاتمه دهند.[۸۱] زنانی هم که قادر به سفر نیستند به ناچار به ارائه دهندگان سقطهای غیرقانونی متوسل میشوند یا اینکه خود تلاش میکنند تا به هر نحوی سقط جنین را انجام دهند.[۸۲] در کشورهایی که سقط جنین بهطور کلی ممنوع نیست، خدمات پیشگیری از بارداری قابل دسترس میباشد و همچنین، گاهی اوقات در کشورهایی هم که سقط جنین در آنها ممنوع است، همچون شیلی، این خدمات دردسترس است.[۸۳][۸۴] این موجب شدهاست تا چالشهایی در رابطه با ساخت اشکال خاصی از قرصهای ضدبارداری اضطراری که موجب سقط جنین میشود، را برای برخی از گروههای حامی زندگی به وجود آورد.
انتخاب جنسیت[ویرایش]
سونوگرافی و آمنیوسنتز به پدر و مادر اجازه میدهد تا از ماهیت جنسیت فرزند خود، قبل از زایمان آگاه شوند. پیشرفت این تکنولوژی به سقط جنینهای انتخابی منجر شدهاست که سقط جنین با توجه به نوع جنسیت رویان انجام میشود، این نوع سقط انتخابی در مورد جنس ماده بسیار شایع است. عنوان میشود که انتخاب جنسی در سقط جنین ممکن است تا حدی مسئول نابرابریهای قابل توجه بین نرخ تولد فرزندان پسر و فرزندان دختر، در بعضی از نقاط جهان باشد. اولویت برای داشتن کودکان پسر و استفاده از سقط جنین برای محدود کردن تولد دختران در بسیاری از نقاط آسیا از جمله چین، تایوان، کره جنوبی و هند گزارش شدهاست.[۸۵] در هند نقش اقتصادی مردان، هزینههای مرتبط با تأمین جهیزیه و همچنین وجود برخی نقشهای فرهنگی سنتی که بر عهده مردان گذاشته شدهاست چون تشییع جنازه توسط خویشاوند نزدیک مرد، منجر به اولویتِ داشتن فرزند پسر به دختر شدهاست.[۸۶] در دسترس بودن گستردهٔ انجام تستهای تشخیصی در طول سالهای ۱۹۷۰ تا ۱۹۸۰ منجر به تبلیغات به منظور سرمایهگذاری در خدماتی گردید که "سرمایهگذاری ۵۰۰ روپیه [برای تشخیص جنسی]، ذخیره ۵۰۰۰۰ روپیه [برای جهیزیه] در آینده "نامیده میشد.[۸۷] در سال ۱۹۹۱ نسبت جنس مرد به زن در هند از هنجار بیولوژیکی خود که ۱۰۵ به ۱۰۰ بود به حدود ۱۰۸ به ۱۰۰ منحرف شد.[۸۸] محققان ادعا میکنند که بین سالهای ۱۹۸۵ و ۲۰۰۵ در حدود ۱۰ میلیون جنین دختر مورد انتخاب سقط جنین قرار گرفته بودند.[۸۹] دولت هند در سال ۱۹۹۴ ممنوعیت سقط جنین انتخابی قبل از وضع حمل را به تصویب رساند و در سال ۲۰۰۲ آن را بهطور رسمی ممنوع اعلام کرد.[۹۰] و در حال حاضر سقط جنین جز در مواردی که سلامتی مادر در خطر باشد، ممنوع است.[۹۰] در جمهوری خلق چین نیز ترجیحِ داشتن فرزند پسر به دختر ریشههای تاریخی دارد. اجرای سیاست تک فرزندی در سال ۱۹۷۹ در پاسخ به نگرانیهای افزایش جمعیت، منجر به افزایش نابرابری در نسبت جنسی شد. این نابرابری در اثر دور زدن قانون، توسط پدر و مادرهایی که از آزادی سقط جنین در جهت سقط جنین دختران ناخواستهشان استفاده میکردند، به وجود میآمد.[۹۱] این احتمال بسیار زیاد است که سقط جنینِ جنس انتخابی، بر روی افزایش نسبت نرخ تولد مرد به زن که ۱۱۷ به ۱۰۰ در سال ۲۰۰۲ گزارش شده، مؤثر بودهاست. این روند بهطور برجستهتری در مناطق روستایی گزارش شده: بالاترین آمار با ۱۳۰ به ۱۰۰ در گوانگدونگ و ۱۳۵ به ۱۰۰ در هاینن بودهاست.[۹۲] ممنوعیت سقط جنین انتخابی در سال ۲۰۰۳ به تصویب رسید[۹۳]
سقط جنین در کشورهای عضو اروپا[ویرایش]
در میان ۲۸ کشور عضو اتحادیه سقط جنین در ۲۴ کشور در هفتههای اول بارداری و اغلب تا پیش از هفته دوازدهم بهطور کامل قانونی است و بنا به درخواست مادر صورت میپذیرد. با این وجود در برخی کشورها همچون ایرلند شمالی، لهستان و فنلاند سقط جنین تنها تحت شرایط خاص صورت میگیرد.[۹۴]
| کشور | بنا به درخواست مادر | به دلایل اقتصادی یا اجتماعی | در صورت وقوع تجاوز | به علت اختلال در سلامت جنین | برای حفظ سلامت جسمانی و روانی مادر | برای حفظ جان مادر |
|---|---|---|---|---|---|---|
| آلمان | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| اتریش | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| اسپانیا | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| استونی | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| اسلوواکی | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| اسلوونی | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| ایتالیا | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| ایرلند | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| بلژیک | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| بلغارستان | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| بریتانیا | در مناطق مختلف متفاوت است. | ✔ | ✔ | ✔ | ✔ | ✔ |
| پرتغال | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| جمهوری چک | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| دانمارک | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| رومانی | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| سوئد | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| فرانسه | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| فنلاند | مجاز نیست | ✔ | ✔ | ✔ | ✔ | ✔ |
| قبرس | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| کرواسی | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| لاتویا | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| لوکزامبورگ | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| لهستان | مجاز نیست | مجاز نیست | ✔ | ✔ | ✔ | ✔ |
| لیتوانی | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| مالتا | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| مجارستان | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| هلند | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
| یونان | ✔ | ✔ | ✔ | ✔ | ✔ | ✔ |
خشونت علیه سقطکنندگان جنین[ویرایش]
مواردی از اعمال خشونت، علیه کسانی که اقدام به انجام سقط جنین میکنند و همچنین ارائهدهندگان امکانات مربوط به سقط جنین، مشاهده شدهاست. خشونت علیه سقط جنین توسط منابع دولتی و علمی به عنوان عملی تروریستی طبقهبندی شدهاست.[۹۵][۹۶] لهستان سقط جنین را ممنوع کرده و این اقدام در روزهای اخیر موجب اعتراض گسترده زنان شدهاست. هزاران زن لهستانی، برای پنجمین روز متوالی در اعتراض به قانون جدید ممنوعیت سقط جنین، به خیابانهای ورشو پایتخت و دیگر شهرهای این کشور آمده و دست به تظاهرات زدند. بر اساس حکم دیوان عالی لهستان، سقط جنین در این کشور، حتی در مواردی چون رشد ناقص جنین نیز بر خلاف قانون اساسی و ممنوع است.[۹۷][۹۸][۹۹]
در ایران[ویرایش]
مشاور دفتر سلامت خانواده وزارت بهداشت در روزنامه وطن امروز، در خرداد ۱۳۹۳ از وقوع روزانه هزار مورد سقط جنین در کشور خبر داد: ۱۵۰ تا ۳۵۰ هزار سقط جنین در طول سال اتفاق میافتد که از این میان ۱۲۰ هزار مورد اعلام کردهاند که فرزند نمیخواستهاند، ۱۰۰ هزار مورد بیمار بودهاند و ۲۰ تا ۳۶ درصد به دلیل مسائل اقتصادی رخ میدهد. محمد اسلامی مشاور فنی دفتر سلامت خانواده وزارت بهداشت با اشاره به سقطهای غیرقانونی در کشور اظهار داشت: ۱۵۰ تا ۳۵۰ هزار سقط جنین در طول سال داریم به طوری که روزانه هزار مورد سقط اتفاق میافتد. وی به دلایل سقط جنین در ایران اشاره کرد و افزود: افزایش سن زن، افزایش سن همسر، فاصله بارداری زیاد پس از ازدواج، بارداری برنامهریزی نشده و تمایل نداشتن به فرزندآوری از این دلایل است و اعتقادات مذهبی مهمترین مانع برای انجام سقط گزارش شدهاند. به گفته اسلامی، از ۲۲۰ هزار مورد در سال ۹۱، ۱۲۰ هزار مورد اعلام کردهاند که فرزند نمیخواستهاند، ۱۰۰ هزار مورد گفتهاند بیمار بودهاند، ۲۰ تا ۳۶ درصد به دلیل مسائل اقتصادی بوده و ۵ درصد به دلیل تداخل با تحصیل گزارش شدهاست.
سقط جنین عمدی از نظر دین اسلام گناه میباشد و حتی در صورتی که جنین حاصل رابطه غیر مشروع باشد نیز این امر را مجاز نمیداند. بنا به نظر اکثر علمای ایران سقط جنین فقط در مواردی که یقین یا خوف خطر جدی وجود داشته باشد مجاز است. برخی از شرایطی که به استناد آن میتوان به صورت قانونی در ایران سقط جنین کرد عبارتند از:
- نطفه در لوله آزمایشگاه رشد یافته باشد.
- در صورتی که جنین ناقصالخلقه شود.
- جان مادر در خطر باشد.
- سلامتی مادر در خطر باشد.
- جنین معیوب یا ناقصالخلقه باشد.
عباس آمیان مدیرکل پزشک قانونی استان کرمان، با اشاره به قانون سقط درمانی مصوب مجلس شورای اسلامی به ایسنا (شهریور ۱۳۹۳) گفت، ماده واحدهٔ سقط درمانی با تشخیص قطعی سه پزشک متخصص و تأیید پزشکی قانونی مبنی بر بیماری جنین که به علت عقبافتادگی یا ناقصالخلقه بودن موجب حرج مادر است یا بیماری مادر که با تهدید جانی مادر توأم باشد پیش از چهار ماه با رضایت زن مجاز به سقط است. وی ادامه داد، در غیر اینصورت متخلفان از اجرای مفاد این قانون به مجازاتهای مقرر در قانون مجازات اسلامی میشوند. مدیرکل پزشک قانونی استان کرمان یادآور شد، پارسال موارد ارجاعی سقط درمانی به ادارهکل پزشکی قانونی ۳۶۷ مورد بودهاست که، نزدیک به ۱۶۷ مورد، منتج به صدور مجوز شدهاند.
شنیده میشود بیشتر مراجعهکنندگان دختران جوانی هستند که بدون اینکه خانوادهٔ آنها چیزی از این ارتباط بدانند مراجعه میکنند.[۱۰۰]
رویکرد به سقط جنین در ادیان[ویرایش]
کلیسای کاتولیک به «حق زندگی» باور دارد و آموزهها و اصول اعتقادی کلیسای کاتولیک در مخالف با عمل «سقط جنین» است.[۱۰۱]
اسلام[ویرایش]
نظرات مسلمانان در مورد سقط جنین توسط حدیث و همچنین نظرات علما و مفسران حقوقی و دینی شکل میگیرد. در اسلام اعتقاد بر این است که جنین پس از ۱۲۰ روز حاملگی به یک جان زنده تبدیل میشود، و سقط جنین پس از آن مرحله غیرمجاز تلقی میشود. بسیاری اسلامی اندیشمندان، استثناهایی را در این قانون برای شرایط خاص تشخیص میدهند. عزیزا یحیی البری، دانشگاهی آمریکایی، خاطرنشان میکند که «اکثر دانشمندان مسلمان سقط جنین را مجاز میدانند، اگرچه نظرشان دربارهٔ مراحل رشد جنین که این امر را ممنوع میکند متفاوت است.» به گفته شرمان جکسون، «در حالی که سقط جنین، حتی در سهماهه اول بارداری، طبق اقلیت حقوقدانان ممنوع است، اما جرمی محسوب نمیشود که مجازات کیفری یا حتی مدنی برای آن در نظر گرفته شده باشد.» چهار مکتب اسلامی سنی وجود دارد.
در عمل، دسترسی به سقط جنین بین کشورهای اکثریت مسلمان بسیار متفاوت است. در کشورهایی مانند ترکیه و تونس، سقط جنین در صورت درخواست، کاملاً قانونی است. از طرف دیگر، در ۱۸ کشور از ۴۷ کشور دارای اکثریت مسلمان، از جمله عراق، مصر و اندونزی، سقط جنین فقط در صورتی مجاز است که زندگی مادر توسط بارداری در خطر باشد. در صورت به خطر افتادن جان مادر، هیچ کشوری با اکثریت مسلمان، سقط جنین را ممنوع نمیکند.
یهودیت[ویرایش]
جستارهای وابسته[ویرایش]
پانویس[ویرایش]
- ^ تعریف علمی سقط جنین عبارتست از: خارج شدن یا تخلیه جنین از رحم قبل از ۵ ماهگی یا وزن جنین زیر ۵۰۰ گرم. Cunningham, FG; Leveno, KJ; Bloom, SL et al, eds. (2010). "1. Overview of Obstetrics". Williams Obstetrics (23 ed.). McGraw-Hill Medical. ISBN 978-0-07-149701-5.
- ^ Premature Birth
- ^ Preterm Birth
- ^ Stillborn
- ^ Suction-Aspiration
منابع[ویرایش]
- ↑ «Domain Registered at Safenames» (PDF). www.thelancetglobalhealthnetwork.com. دریافتشده در ۲۰۲۴-۰۱-۱۷.
- ↑ ۲٫۰ ۲٫۱ ۲٫۲ ۲٫۳ Shah, I. ; Ahman, E. (December 2009). "Unsafe abortion: global and regional incidence, trends, consequences, and challenges" (PDF). Journal of Obstetrics and Gynaecology Canada 31 (12): 1149–58. PMID 20085681
- ↑ ۳٫۰ ۳٫۱ Culwell KR, Vekemans M, de Silva U, Hurwitz M (July 2010). "Critical gaps in universal access to reproductive health: Contraception and prevention of unsafe abortion". International Journal of Gynecology & Obstetrics 110: S13–16. doi:10.1016/j.ijgo.2010.04.003. PMID 20451196
- ↑ Sedgh G, Henshaw SK, Singh S, Bankole A, Drescher J (September 2007). "Legal abortion worldwide: incidence and recent trends". Int Fam Plan Perspect 33 (3): 106–16. doi:10.1363/ifpp.33.106.07. PMID 17938093
- ↑ ۵٫۰ ۵٫۱ خطای یادکرد: خطای یادکرد:برچسب
<ref> غیرمجاز؛ متنی برای یادکردهای با نامhdl.handle.netوارد نشده است. (صفحهٔ راهنما را مطالعه کنید.). - ↑ # ^ http://www.bbc.co.uk/religion/religions/islam/islamethics/abortion_1.shtml
- ↑ Dabash, Rasha; Roudi-Fahimi, Farzaneh (2008). "Abortion in the Middle East and North Africa" (PDF). Population Research Bureau. Archived from the original on July 8, 2011. http://www.prb.org/pdf08/MENAabortion.pdf بایگانیشده در ۲۰۱۱-۱۰-۰۶ توسط Wayback Machine.
- ↑ ۸٫۰ ۸٫۱ ۸٫۲ # Brind'Amour, Katherine (2007). "Effraenatam". Embryo Project Encyclopedia. Arizona State University. http://hdl.handle.net/2286/embryo:124802.
- ↑ ۹٫۰ ۹٫۱ ^ "Abortion Law, History & Religion". Childbirth By Choice Trust. Archived from the original on 2008-02-08. https://web.archive.org/web/20080208053146/http://www.cbctrust.com/history_law_religion.php. Retrieved 2008-03-23.
- ↑ # ^ Brind'Amour, Katherine (2007). "Effraenatam". Embryo Project Encyclopedia. Arizona State University. http://hdl.handle.net/2286/embryo:124802.
- ↑ ^ World Abortion Policies 2007, United Nations, Department of Economic and Social Affairs, Population Division.
- ↑ ^ Theodore J. Joyce, Stanley K. Henshaw, Amanda Dennis, Lawrence B. Finer and Kelly Blanchard (April 2009). "The Impact of State Mandatory Counseling and Waiting Period Laws on Abortion: A Literature Review" (PDF). Guttmacher Institute. Archived from the original on 2011-01-14. https://web.archive.org/web/20120316155239/http://internationalfamilyplanningperspectives.org/pubs/MandatoryCounseling.pdf. Retrieved December 31, 2010.
- ↑ Cheng L. (November 1, 2008). "Surgical versus medical methods for second-trimester induced abortion". The WHO Reproductive Health Library. World Health Organization. Archived from the original on June 17, 2011. http://apps.who.int/rhl/fertility/abortion/CD006714_chengl_com/en/index.html. Retrieved June 17, 2011.
- ↑ Bankole et al. , "Reasons Why Women Have Induced Abortions: Evidence from 27 Countries", International Family Planning Perspectives (1998). Also see Lawrence B. Finer, Lori F. Frohwirth, Lindsay A. Dauphinee, Susheela Singh, and Ann M. Moore, "Reasons U.S. Women Have Abortions: Quantitative and Qualitative Perspectives", Perspectives on Sexual and Reproductive Health, 37(3):110-118 (September 2005).
- ↑ # Stubblefield, Phillip G. (2002). "10. Family Planning". In Berek, Jonathan S.. Novak's Gynecology (13 ed.). Lippincott Williams & Wilkins. ISBN 978-0-7817-3262-8. # ^ Menikoff, Jerry (2001). Law and Bioethics. Georgetown University Press. p. 78. ISBN 978-0-87840-839-9. http://books.google.com/books?id=2jXOYv3X8zsC&pg=PA78. "As the fetus grows in size, however, the vacuum aspiration method becomes increasingly difficult to use."
- ↑ ۱۶٫۰ ۱۶٫۱ Roche, Natalie E. (September 28, 2004). "Therapeutic Abortion". eMedicine. Archived from the original on December 14, 2004. https://web.archive.org/web/20041214092044/http://www.emedicine.com/MED/topic3311.htm. Retrieved June 19, 2011
- ↑ Schorge, John O. ; Schaffer, Joseph I. ; Halvorson, Lisa M. et al. , eds (2008). "6. First-Trimester Abortion". Williams Gynecology (1 ed.). McGraw-Hill Medical. ISBN 978-0-07-147257-9
- ↑ Annas, George J. ; Elias, Sherman (2007). "51. Legal and Ethical Issues in Obstetric Practice". In Gabbe, Steven G. ; Niebyl, Jennifer R. ; Simpson, Joe Leigh. Obstetrics: Normal and Problem Pregnancies (5 ed.). Churchill Livingstone. p. 669. ISBN 978-0-443-06930-7. "A preterm birth is defined as one that occurs before the completion of 37 menstrual weeks of gestation, regardless of birth weight.
- ↑ "Stillbirth". Concise Medical Dictionary. Oxford University Press. 2010. "birth of a fetus that shows no evidence of life (heartbeat, respiration, or independent movement) at any time later than 24 weeks after conception"
- ↑ Annas, George J. ; Elias, Sherman (2007). "24. Pregnancy loss". In Gabbe, Steven G. ; Niebyl, Jennifer R. ; Simpson, Joe Leigh. Obstetrics: Normal and Problem Pregnancies (5 ed.). Churchill Livingstone. ISBN 978-0-443-06930-7.
- ↑ Schorge, John O. ; Schaffer, Joseph I. ; Halvorson, Lisa M. et al. , eds (2008). "6. First-Trimester Abortion". Williams Gynecology (1 ed.). McGraw-Hill Medical. ISBN 978-0-07-147257-9.
- ↑ Katz, Vern L. (2007). "16. Spontaneous and Recurrent Abortion - Etiology, Diagnosis, Treatment". In Katz, Vern L. ; Lentz, Gretchen M. ; Lobo, Rogerio A. et al.. Katz: Comprehensive Gynecology (5 ed.). Mosby. ISBN 978-0-323-02951-3.
- ↑ Stöppler, Melissa Conrad. "Miscarriage (Spontaneous Abortion)". In Shiel, William C. , Jr.. MedicineNet.com. WebMD. http://www.medicinenet.com/miscarriage/page1.htm. Retrieved 2009-04-07.
- ↑ Jauniaux E, Kaminopetros P, El-Rafaey H (1999). "Early pregnancy loss". In Whittle MJ, Rodeck CH. Fetal medicine: basic science and clinical practice. Edinburgh: Churchill Livingstone. p. 837. ISBN 978-0-443-05357-3. OCLC 42792567. http://books.google.com/?id=0BY0hx2l5uoC[پیوند مرده].
- ↑ "Fetal Homicide Laws". National Conference of State Legislatures. http://www.ncsl.org/programs/health/fethom.htm بایگانیشده در ۱۱ سپتامبر ۲۰۱۲ توسط Archive.today. Retrieved 2009-04-07.
- ↑ Thapa, S. R. ; Rimal, D. ; Preston, J. (2006). "Self induction of abortion with instrumentation". Australian Family Physician 35 (9): 697–698. PMID 16969439
- ↑ Grimes, DA; Creinin, MD (2004). "Induced abortion: an overview for internists". Ann. Intern. Med. 140 (8): 620–6. doi:10.1001/archinte.140.5.620. PMID 15096333
- ↑ Grimes DA (January 2006). "Estimation of pregnancy-related mortality risk by pregnancy outcome, United States, 1991 to 1999". Am. J. Obstet. Gynecol. 194 (1): 92–4. doi:10.1016/j.ajog.2005.06.070. PMID 16389015
- ↑ Bartlett LA, Berg CJ, Shulman HB et al. (April 2004). "Risk factors for legal induced abortion-related mortality in the United States". Obstet Gynecol 103 (4): 729–37. doi:10.1097/01.AOG.0000116260.81570.60. PMID 15051566
- ↑ Trupin, Suzanne (May 27, 2010). "Elective Abortion". eMedicine. http://emedicine.medscape.com/article/252560-overview. Retrieved June 1, 2010. "At every gestational age, elective abortion is safer for the mother than carrying a pregnancy to term."
- ↑ Westfall JM, Sophocles A, Burggraf H, Ellis S (1998). "Manual vacuum aspiration for first-trimester abortion". Arch Fam Med 7 (6): 559–62. doi:10.1001/archfami.7.6.559. PMID 9821831
- ↑ ACOG Committee on Practice Bulletins--Gynecology (May 2009). "ACOG practice bulletin No. 104: antibiotic prophylaxis for gynecologic procedures". Obstet Gynecol 113 (5): 1180–9. doi:10.1097/AOG.0b013e3181a6d011. PMID 19384149
- ↑ Sawaya GF, Grady D, Kerlikowske K, Grimes DA (May 1996). "Antibiotics at the time of induced abortion: the case for universal prophylaxis based on a meta-analysis". Obstet Gynecol 87 (5 Pt 2): 884–90. PMID 8677129
- ↑ Lohr PA, Hayes JL, Gemzell-Danielsson K (2008). Lohr, Patricia A.. ed. "Surgical versus medical methods for second trimester induced abortion". Cochrane Database Syst Rev (1): CD006714.
- ↑ Spitz IM, Bardin CW, Benton L, Robbins A (April 1998). "Early pregnancy termination with mifepristone and misoprostol in the United States". N. Engl. J. Med. 338 (18): 1241–7. doi:10.1056/NEJM199804303381801. PMID 956257
- ↑ Aubény E, Peyron R, Turpin CL et al. (1995). "Termination of early pregnancy (up to 63 days of amenorrhea) with mifepristone and increasing doses of misoprostol[corrected]". Int J Fertil Menopausal Stud 40 Suppl 2: 85–91. PMID 8574255
- ↑ ^ "Medical versus surgical methods for first trimester termination of pregnancy". World Health Organization. December 15, 2006. http://apps.who.int/rhl/fertility/abortion/pccom/en/index.html. Retrieved June 1, 2010.
- ↑ Spitz IM, Bardin CW, Benton L, Robbins A (April 1998). "Early pregnancy termination with mifepristone and misoprostol in the United States". N. Engl. J. Med. 338 (18): 1241–7. doi:10
- ↑ Fischer M, Bhatnagar J, Guarner J et al. (December 2005). "Fatal toxic shock syndrome associated with Clostridium sordellii after medical abortion". N. Engl. J. Med. 353 (22): 2352–60. doi:10.1056/NEJMoa051620. PMID 16319384
- ↑ ^ Fjerstad M, Trussell J, Sivin I, Lichtenberg ES, Cullins V (July2009). "Rates of serious infection after changes in regimens for medical abortion". N. Engl. J. Med. 361 (2): 145–51. doi:10.1056/NEJMoa0809146. PMID 19587339
- ↑ ^ Haddad, LB. ; Nour, NM. (2009). "Unsafe abortion: unnecessary maternal mortality". Rev Obstet Gynecol 2 (2): 122–6. PMC 2709326. PMID 19609407
- ↑ Grimes DA, Benson J, Singh S et al. (2006). "Unsafe abortion: the preventable pandemic" (PDF). Lancet 368 (9550): 1908–19. doi:10.1016/S0140-6736(06)69481-6. PMID 17126724
- ↑ Berer M (November 2004). "National laws and unsafe abortion: the parameters of change". Reprod Health Matters 12 (24 Suppl): 1–8. doi:10.1016/S0968-8080(04)24024-1. PMID 15938152
- ↑ ۴۴٫۰ ۴۴٫۱ Berer M (2000). "Making abortions safe: a matter of good public health policy and practice". Bull. World Health Organ. 78 (5): 580–92. PMC 2560758. PMID 10859852
- ↑ Jewkes R, Rees H, Dickson K, Brown H, Levin J (March 2005). "The impact of age on the epidemiology of incomplete abortions in South Africa after legislative change". BJOG 112 (3): 355–9. doi:10.1111/j.1471-0528.2004.00422.x. PMID 15713153
- ↑ Bateman C (December 2007). "Maternal mortalities 90% down as legal TOPs more than triple". S. Afr. Med. J. 97 (12): 1238–42. PMID 18264602
- ↑ ۴۷٫۰ ۴۷٫۱ Jasen P (2005). "Breast cancer and the politics of abortion in the United States". Medical History 49 (4): 423–44. PMC 1251638. PMID 16562329
- ↑ # World Health Organization: "Induced abortion does not increase breast cancer risk (Fact sheet N°240)". World Health Organization. Archived from the original on February 13, 2011. https://web.archive.org/web/20110213141046/http://www.who.int/mediacentre/factsheets/fs240/en/. Retrieved January 6, 2011. # National Cancer Institute: "Abortion, Miscarriage, and Breast Cancer Risk". National Cancer Institute. http://www.cancer.gov/cancertopics/factsheet/risk/abortion-miscarriage. Retrieved January 11, 2011. # American Cancer Society: "Is Abortion Linked to Breast Cancer?". American Cancer Society. September 23, 2010. http://www.cancer.org/Cancer/BreastCancer/MoreInformation/is-abortion-linked-to-breast-cancer بایگانیشده در ۵ ژوئن ۲۰۱۱ توسط Wayback Machine. Retrieved June 20, 2011. "At this time, the scientific evidence does not support the notion that abortion of any kind raises the risk of breast cancer." # Royal College of Obstetricians and Gynaecologists: "The Care of Women Requesting Induced Abortion" (PDF). Royal College of Obstetricians and Gynaecologists. p. 9. http://www.rcog.org.uk/files/rcog-corp/uploaded-files/NEBAbortionSummary.pdf بایگانیشده در ۲۷ ژوئیه ۲۰۱۳ توسط Wayback Machine. Retrieved June 29, 2008. "Induced abortion is not associated with an increase in breast cancer risk." # American Congress of Obstetricians and Gynecologists: "ACOG Finds No Link Between Abortion and Breast Cancer Risk". American Congress of Obstetricians and Gynecologists. July 31, 2003. http://www.acog.org/from_home/publications/press_releases/nr07-31-03-2.cfm بایگانیشده در ۲ ژانویه ۲۰۱۱ توسط Wayback Machine. Retrieved January 11, 2011.
- ↑ ^ "APA Task Force Finds Single Abortion Not a Threat to Women's Mental Health" (Press release). American Psychological Association. August 12, 2008. http://www.apa.org/news/press/releases/2008/08/single-abortion.aspx. Retrieved September 7, 2011.
- ↑ ^ "Report of the APA Task Force on Mental Health and Abortion". Washington, DC: American Psychological Association. August 13, 2008. http://www.apa.org/pi/women/programs/abortion/mental-health.pdf.
- ↑ Culwell KR, Vekemans M, de Silva U, Hurwitz M (July 2010). "Critical gaps in universal access to reproductive health: Contraception and prevention of unsafe abortion". International Journal of Gynecology & Obstetrics 110: S13–16. doi:10.1016/j.ijgo.2010.04.003. PMID 20451196.
- ↑ Rosenthal, Elizabeth (October 12, 2007). "Legal or Not, Abortion Rates Compare". The New York Times. http://www.nytimes.com/2007/10/12/world/12abortion.html?. Retrieved July 18, 2011. "Anti-abortion groups criticized the research, saying that the scientists had jumped to conclusions from imperfect tallies, often estimates of abortion rates in countries where the procedure was illegal.
- ↑ Henshaw, Stanley K. , Singh, Susheela, and Haas, Taylor. (1999). The Incidence of Abortion Worldwide. International Family Planning Perspectives, 25 (Supplement), 30–38. Retrieved 2006-01-18.
- ↑ Strauss, L.T. , Gamble, S.B. , Parker, W.Y, Cook, D.A. , Zane, S.B. , and Hamdan, S. (November 24, 2006). Abortion Surveillance – United States, 2003. Morbidity and Mortality Weekly Report, 55 (11), 1–32. Retrieved May 10, 2007.
- ↑ "The Limitations of U.S. Statistics on Abortion". Issues in Brief. New York: The Guttmacher Institute. 1997. http://www.guttmacher.org/pubs/ib14.html بایگانیشده در ۴ آوریل ۲۰۱۲ توسط Wayback Machine.
- ↑ ۵۶٫۰ ۵۶٫۱ ۵۶٫۲ «جانور غالب»: جلد هفتم (فراز و نشیب جمعیتها)- اثر پل ارلیک، آن ارلیک- ترجمهٔ آرش حسینیان- نشر اینترنتی- چاپ اول 1393- ص20
- ↑ ژنتیک عامل 70 درصد کل سقطها در جهان.[خبرگزاری جمهوری اسلامی(ایرنا) http://www.irna.ir]
- ↑ Finer, L. B. ; Henshaw, S. K. (2003). "Abortion Incidence and Services in the United States in 2000". Perspectives on Sexual and Reproductive Health 35 (1): 6–15. doi:10.1363/3500603. PMID 12602752
- ↑ Department of Health (2007). "Abortion statistics, England and Wales: 2006". http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsStatistics/DH_075697 بایگانیشده در ۶ دسامبر ۲۰۱۰ توسط Wayback Machine. Retrieved 2007-10-12.
- ↑ Cheng L. “Surgical versus medical methods for second-trimester induced abortion: RHL commentary” (last revised: November 1, 2008). The WHO Reproductive Health Library; Geneva: World Health Organization.
- ↑ # Bankole, Akinrinola, Singh, Susheela, and Haas, Taylor. (1998). Reasons Why Women Have Induced Abortions: Evidence from 27 Countries. International Family Planning Perspectives, 24 (3), 117–127 and 152. Retrieved 2006-01-18.
- ↑ ۶۲٫۰ ۶۲٫۱ Jones, R. K. ; Darroch, J. E. ; Henshaw, S. K. (2002). "Contraceptive Use Among U.S. Women Having Abortions in 2000-2001" (PDF). Perspectives on Sexual and Reproductive Health 34 (6): 294–303. doi:10.2307/3097748. PMID 12558092. http://www.guttmacher.org/pubs/journals/3429402.pdf.
- ↑ ۶۳٫۰ ۶۳٫۱ Susan A. Cohen: Abortion and Women of Color: The Bigger Picture, Guttmacher Policy Review, Summer 2008, Volume 11, Number 3.
- ↑ Department of Health (2007). "Abortion statistics, England and Wales: 2006". http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsStatistics/DH_075697 بایگانیشده در ۶ دسامبر ۲۰۱۰ توسط Wayback Machine. Retrieved 2007-10-12
- ↑ Maclean, Gaynor. "Dimension, Dynamics and Diversity; A 3D Approach to Appraising Global Maternal and Neonatal Health Initiatives", pages 299-300 in Trends in Midwifery Research by Randell Balin (Nova Publishers, 2005).
- ↑ World Health Organization. (2004). "Unsafe abortion: global and regional estimates of unsafe abortion and associated mortality in 2000". Retrieved 2009-03-22.
- ↑ Sedgh G, Henshaw S, Singh S, Ahman E, Shah IH (2007). "Induced abortion: estimated rates and trends worldwide". Lancet 370 (9595): 1338–45. doi:10.1016/S0140-6736(07)61575-X. PMID 17933648
- ↑ "Unsafe abortion: Global and regional estimates of the incidence of unsafe abortion and associated mortality in 2003" (PDF). World Health Organization. 2007. http://whqlibdoc.who.int/publications/2007/9789241596121_eng.pdf. Retrieved March 7, 2011.
- ↑ Singh, Susheela et al. Adding it Up: The Costs and Benefits of Investing in Family Planning and Newborn Health (New York: Guttmacher Institute and United Nations Population Fund 2009): "If women’s contraceptive needs were addressed (and assuming no changes in abortion laws)...the number of unsafe abortions would decline by 73% from 20 million to 5.5 million." A few of the findings in that report were subsequently changed, and are available at: "Facts on Investing in Family Planning and Maternal and Newborn Health" (Guttmacher Institute 2010).
- ↑ Salter, C. , Johnson, H.B. , and Hengen, N. (1997). "Care for Postabortion Complications: Saving Women's Lives". Population Reports (Johns Hopkins School of Public Health) 25 (1). Archived from the original on September 1, 2011. http://www.webcitation.org/61MhmDwmL بایگانیشده در ۱۸ ژانویه ۲۰۱۲ توسط Wayback Machine.
- ↑ UNICEF, United Nations Population Fund, WHO, World Bank (2010). "Packages of interventions: Family planning, safe abortion care, maternal, newborn and child health". http://www.who.int/reproductivehealth/publications/maternal_perinatal_health/fch_10_06/en/index.html. Retrieved December 31, 2010.
- ↑ Shah, I. ; Ahman, E. (December 2009). "Unsafe abortion: global and regional incidence, trends, consequences, and challenges" (PDF). Journal of Obstetrics and Gynaecology Canada 31 (12): 1149–58. PMID 20085681. http://www.sogc.org/jogc/abstracts/full/200912_WomensHealth_1.pdf بایگانیشده در ۱۶ ژوئیه ۲۰۱۱ توسط Wayback Machine.
- ↑ offe, Carole (2009). "1. Abortion and medicine: A sociopolitical history". In MPaul, ES Lichtenberg, L Borgatta, DA Grimes, PG Stubblefield, MD Creinin. Management of Unintended and Abnormal Pregnancy (1st ed.). Oxford, United Kingdom: John Wiley & Sons, Ltd.. p. 2. ISBN 978-1-4443-1293-5
- ↑ alter, C. , Johnson, H.B. , and Hengen, N. (1997). "Care for Postabortion Complications: Saving Women's Lives". Population Reports (Johns Hopkins School of Public Health) 25 (1). Archived from the original on September 1, 2011. http://www.webcitation.org/61MhmDwmL بایگانیشده در ۱۸ ژانویه ۲۰۱۲ توسط Wayback Machine.
- ↑ Singh, Susheela et al. Adding it Up: The Costs and Benefits of Investing in Family Planning and Newborn Health (New York: Guttmacher Institute and United Nations# Population Fund 2009): "If women’s contraceptive needs were addressed (and assuming no changes in abortion laws)...the number of unsafe abortions would decline by 73% from 20 million to 5.5 million." A few of the findings in that report were subsequently changed, and are available at: "Facts on Investing in Family Planning and Maternal and Newborn Health" (Guttmacher Institute 2010).
- ↑ Miles, Steven (2005). The Hippocratic Oath and the Ethics of Medicine. Oxford University Press. ISBN 978-0-19-518820-2
- ↑ ^ "Nicaragua: "The Women’s Movement Is in Opposition"". IPS. Montevideo: Inside Costa Rica. June 28, 2008. http://insidecostarica.com/special_reports/2008-06/nicaragua_womens_movement.htm.
- ↑ "Surgical Abortion: History and Overview". National Abortion Federation. http://www.prochoice.org/education/resources/surg_history_overview.html بایگانیشده در ۲۲ سپتامبر ۲۰۰۶ توسط Wayback Machine. Retrieved 2006-09-04.
- ↑ Henshaw, S. K. (1991). "The Accessibility of Abortion Services in the United States". Family Planning Perspectives 23 (6): 246–263. doi:10.2307/2135775
- ↑ Marcy Bloom (February 25, 2008). "Need Abortion, Will Travel". RH Reality Check. http://www.rhrealitycheck.org/blog/2008/02/25/need-abortion-will-travel. Retrieved 2009-06-15.
- ↑ Ross, Jen (September 12, 2006). "In Chile, free morning-after pills to teens". The Christian Science Monitor. http://www.csmonitor.com/2006/0912/p01s04-woam.html. Retrieved 2006-12-07
- ↑ Gallardoi, Eduardo (September 26, 2006). "Morning-After Pill Causes Furor in Chile". The Washington Post. http://www.washingtonpost.com/wp-dyn/content/article/2006/09/26/AR2006092600770.html. Retrieved 2006-12-07
- ↑ Banister, Judith. (1999-03-16). Son Preference in Asia – Report of a Symposium. Retrieved 2006-01-12
- ↑ Mutharayappa, Rangamuthia, Kim Choe, Minja, Arnold, Fred, and Roy, T.K. (1997). Son Preferences and Its Effect on Fertility in India. National Family Health Survey Subject Reports, Number 3. '. ' Retrieved 2006-01-12.
- ↑ Patel, Rita (Fall 1996). "The practice of sex selective abortion in India: May you be the mother of a hundred sons" (PDF). Carolina Papers in International Health and Development 7. Archived from the original on 2010-06-16. https://web.archive.org/web/20100612101835/http://cgi.unc.edu/research/pdf/abortion.pdf. Retrieved 2008-12-03.
- ↑ Sudha, S. ; Rajan, S. Irudaya (July 1999). "Female Demographic Disadvantage in India 1981–1991: Sex Selective Abortions and Female Infanticide". Development and Change 30 (3): 585–618. doi:10.1111/1467-7660.00130. PMID 20162850. Archived from the original on 2003-01-01. https://web.archive.org/web/20030101210623/http://www.hsph.harvard.edu/organizations/healthnet/gender/docs/sudha.html. Retrieved 2008-12-03
- ↑ Reaney, Patricia. "Selective abortion blamed for India's missing girls". Reuters. Archived from the original on 2006-02-20. https://web.archive.org/web/20060220072756/http://www.alertnet.org/thenews/newsdesk/L06779563.htm. Retrieved 2008-12-03.
- ↑ # "Sex Selection & Abortion: India". Library of Congress. April 4, 2011. http://www.loc.gov/law/help/sex-selection/india.php. Retrieved July 18, 2011.
- ↑ Graham, Maureen J. ; Larsen; Xu (June 1998). "Son Preference in Anhui Province, China". International Family Planning Perspectives 24 (2): 72–77. doi:10.2307/2991929. Archived from the original on June 20, 2008. https://web.archive.org/web/20080620084622/http://www.agi-usa.org/pubs/journals/2407298.html. Retrieved 2008-12-03
- ↑ ۹۰٫۰ ۹۰٫۱ # Plafker, Ted (May 2002). "Sex selection in China sees 117 boys born for every 100 girls". BMJ 324 (7348): 1233a. doi:10.1136/bmj.324.7348.1233/a. PMC 1123206. PMID 12028966. http://www.pubmedcentral.nih.gov/articlerender.fcgi?tool=pmcentrez&artid=1123206.
- ↑ "China Bans Sex-selection Abortion." (2002-03-22). Xinhua News Agency. '. ' Retrieved 2006-01-12.
- ↑ # Smith, G. Davidson (Tim) (1998). "Single Issue Terrorism Commentary". Canadian Security Intelligence Service. Archived from the original on October 15, 2007. https://web.archive.org/web/20071015065711/http://csis-scrs.gc.ca/en/publications/commentary/com74.asp. Retrieved September 1, 2011. # ^
- ↑ Wilson, M. ; Lynxwiler, J. (1988). "Abortion clinic violence as terrorism". Studies in Conflict & Terrorism 11 (4): 263–273. doi:10.1080/10576108808435717
- ↑ http://fa.euronews.com/2018/05/24/rish-abortion-referendum-and-rules-in-other-eu-states
- ↑ "The Death of Dr. Gunn". New York Times. March 12, 1993. http://www.nytimes.com/1993/03/12/opinion/the-death-of-dr-gunn.html.
- ↑ "Incidence of Violence & Disruption Against Abortion Providers in the U.S. & Canada" (PDF). National Abortion Federation. 2009. http://www.prochoice.org/pubs_research/publications/downloads/about_abortion/violence_stats.pdf. Retrieved February 9, 2010.
- ↑ 1787 (۲۰۲۰-۱۰-۲۷). «ادامه تظاهرات علیه قانون ممنوعیت سقط جنین در لهستان». ایرنا. دریافتشده در ۲۰۲۰-۱۰-۳۱.
- ↑ 1385 (۲۰۲۰-۱۰-۳۱). «هزاران نفر علیه قانون ممنوعیت سقط جنین در لهستان تظاهرات کردند». ایرنا. دریافتشده در ۲۰۲۰-۱۰-۳۱.
- ↑ «هزاران لهستانی در اعتراض به محدود شدن سقط جنین به خیابان آمدند». BBC News فارسی. دریافتشده در ۲۰۲۰-۱۰-۳۱.
- ↑ «آمار سیاه پروندههای سقط جنین در کرمان». ایسنا. ۲۰۱۴-۰۹-۰۲. دریافتشده در ۲۰۱۴-۰۹-۰۲.
- ↑ تلاش واتیکان و سازمان راهبههای آمریکایی برای تفاهم، بیبیسی فارسی
